Ventriculomegaly
Ventriculomegaly is the enlargement of the cerebral ventricles with the cause unknown. The term hydrocephalus is usually reserved for more severe cases of ventriculomegaly, and this usually implies obstruction of flow of the CSF. Obstructive hydrocephalus within the fetus is most commonly non-communicating (blockage within ventricles) rather than communicating (extraventricular blockage). Moreover, underdevelopment of the brain and destructive brain lesions can also cause ventriculomegaly.
Brain destruction is another cause of ventriculomegaly and may include in utero damage due to a CNS infection. CNS infections may be associated with brain atrophy, with resultant microcephaly and ventriculomegaly.
The main causes of fetal ventriculomegaly are aqueductal stenosis, Chiari II malformation, Dandy-Walker complex and agenesis of the corpus callosum.
Fig1, Fig2, Fig3, Fig4
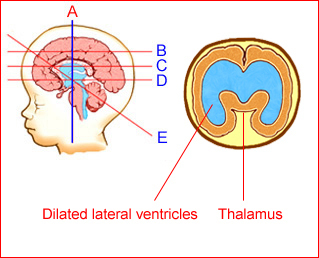
Fig1: Schematic drawing: Coronal view: Ventriculomegaly with wide separation of the thalami
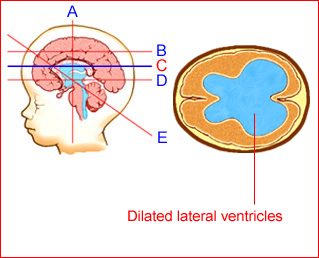
Fig 2: Schematic drawing: Transventricular view: Ventriculomegaly secondary to aqueductal stenosis
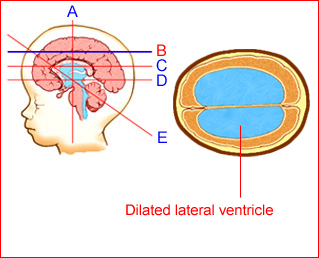
Fig 3: Schematic drawing: Transventricular view: Ventriculomegaly secondary to aqueductal stenosis
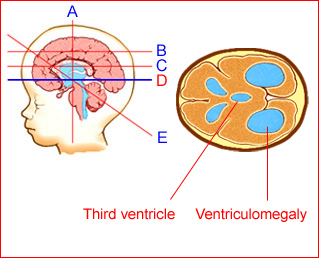
Fig 4: Schematic drawing: Transthalamic view: Ventriculomegaly with dilated third ventricle secondary to aqueductal stenosis
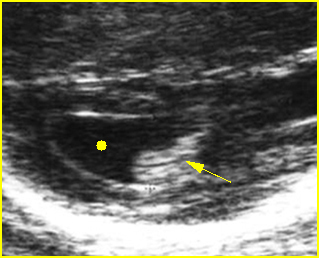
Fig 5: Mild ventriculomegaly Lateral ventricle (solid circle), width of 11 mm, with choroid plexus dangling sign (arrow)
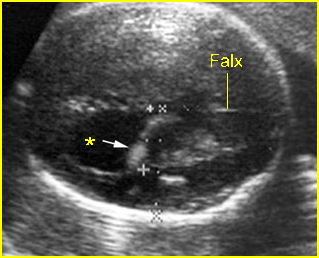
Fig 6: Ventriculomegaly Lateral ventricle (*), width of 15 mm, with choroid plexus dangling sign (arrow)
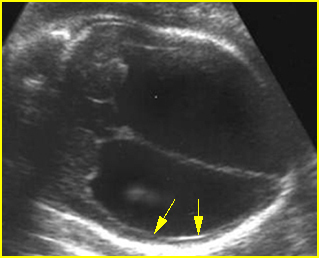
Fig 7: Severe hydrocephalus Markedly dilated ventricles with extremely thin brain (arrow)
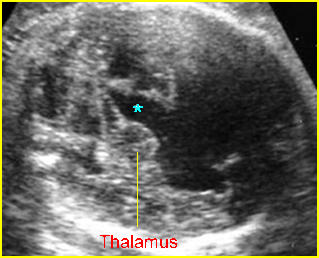
Fig 8: Hydrocephalus Transthalamic view: wide separation the third ventricle (*) and dilated lateral ventricles
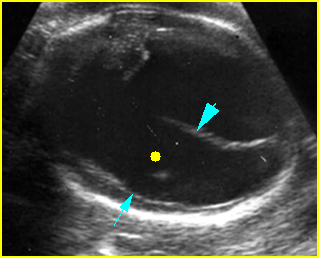
Fig 9: Severe hydrocephalus Markedly dilated ventricles (solid circle) with extremely thin brain (arrow), (arrowhead = falx cerebri)
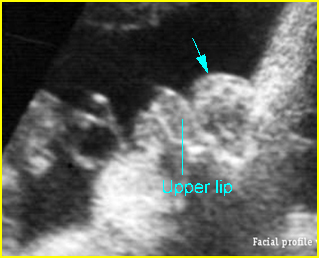
Fig 10: Bossing forehead secondary to hydrocephaly Facial profile view: sunken nose related to forehead bossing in case of hydrocephaly
Mild (borderline) ventriculomegaly [Fig5, Fig6] is used when the atrial width is 10-15 mm. Some consider early ventricular dilatation as separation (>3 mm) of the dependent choroid from the medial ventricular wall. This occurs bilaterally in 0.15-0.7% of fetuses and unilaterally in 0.07% of pregnancies. This can be related to an increased risk of CNS and non-CNS anomalies. Isolated borderline ventriculomegaly is normal variant in most cases, however, it may represent the earliest manifestation of cerebral anomalies (4%), chromosomal abnormalities (4%) (mostly trisomy 21) and overall abnormal outcomes (20%).
However, early and unexplained mild ventriculomegaly appears to have a good prognosis but a long postnatal clinical follow-up is required.
Overt (or moderate to severe) ventriculomegaly [Fig7, Fig8, Fig9, Fig10] is usually defined for an atrial width of more than 15 mm in the second and third trimesters(8). This may involve isolated cases (30-60%) or cases associated with other CNS anomalies, most frequently neural tube defects (NTDs) and midline defects. The degree of antenatal ventriculomegaly is related to pediatric neurological morbidity and, when it is >15 mm, it is associated with an increase in abnormal neurological development.
Unilateral ventriculomegaly is a rare finding usually due to focal obstruction of the CSF pathway at the level of Monro’s foramen. Examination of the lateral ventricles using the angled technique helps to distinguish between unilateral and bilateral hydrocephalus. Unilateral ventriculomegaly is usually an isolated finding and when isolated has little measurable effect on developmental outcome.
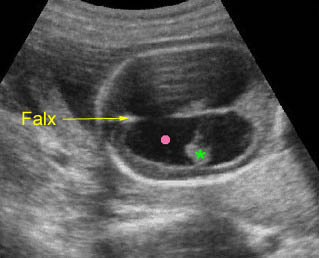
Hydrocephalus: Transverse scan of the head: markedly dilated ventricles (solid circle) with very thin cerebral tissue (* = dangling choroid plexus)
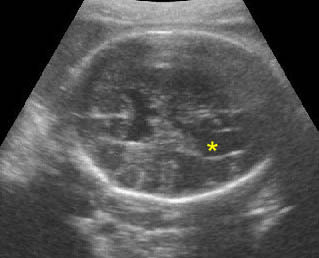
Mild ventriculomegaly: Transverse scan of the head: lateral ventricle (*) width of 10 mm diameter
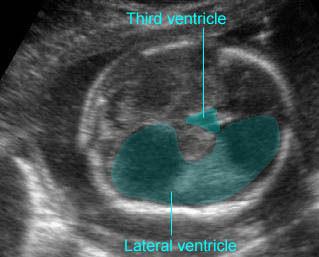
Hydrocephaly: Overt ventriculomegaly with dilatation of the third ventricle
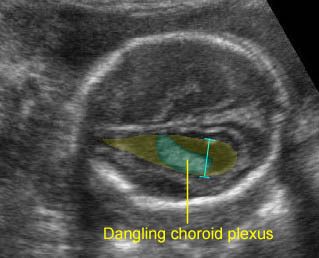
Mild ventriculomegaly: Transventricular view: mild dilatation of the lateral ventricle (10 mm.) with dangling choroid plexus
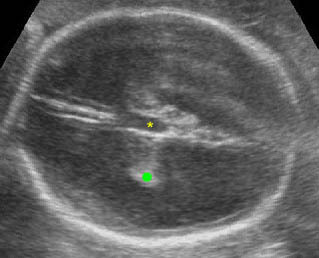
Severe hydrocephalus: Transverse scan of the head: markedly dilated ventricles with extremely thin cerebral tissue (solid circle = dangling choroid plexus, * = dilated third ventricle)
Sonographic findings:
- Enlargement of the lateral ventricle atrium >10 mm.
- Minimal separation of the choroid plexus in either proximal or distal cerebral ventricle.
- Dangling choroid plexus with an abnormal choroid angle (more than 29 degrees)(14). Dangling can be easily recognized without measuring it in most cases.
- When ventriculomegaly is detected, a careful anatomic survey of the fetus is necessary to determine any associated anomalies. Furthermore, hydrocephalus is associated with a significant risk of chromosomal abnormalities. When objective difficulties preclude detailed sonographic examination, MRI is helpful(15).
- Sonographic differential diagnoses of ventriculomegaly include
- Arnold-Chiari malformation type II:
- deformed cranium (lemon sign), which usually disappears in the third trimester
- obliteration of cisterna magna (banana sign)
- associated open spinal defect
- minimal hydrocephalus
- pointed frontal horns
- Dandy-Walker malformation:
- midline posterior fossa cyst
- cyst communicates with the fourth ventricle
- vermian agenesis
- hypoplastic cerebellar hemispheres
- elevated tentorium
- mild to moderate hydrocephalus
- Agenesis of the corpus callosum:
- third ventricle elevated
- separation of frontal horns
- associated colpocephaly
- mild ventriculomegaly
- Aqueduct stances:
- moderate to massive hydrocephalus
- normal fourth ventricle
- normal posterior fossa
- normal cranial configuration
- Cephalocele:
- open defect, usually occipital skull base
- obliteration of the cisterna magna
- occasional lemon sign
- mild to moderate hydrocephalus
- polyhydramnios.
- Arnold-Chiari malformation type II:

